Research analysis on fertility plunged 23% reveals how healthcare leaders can grow with ethical IVF strategy insights.
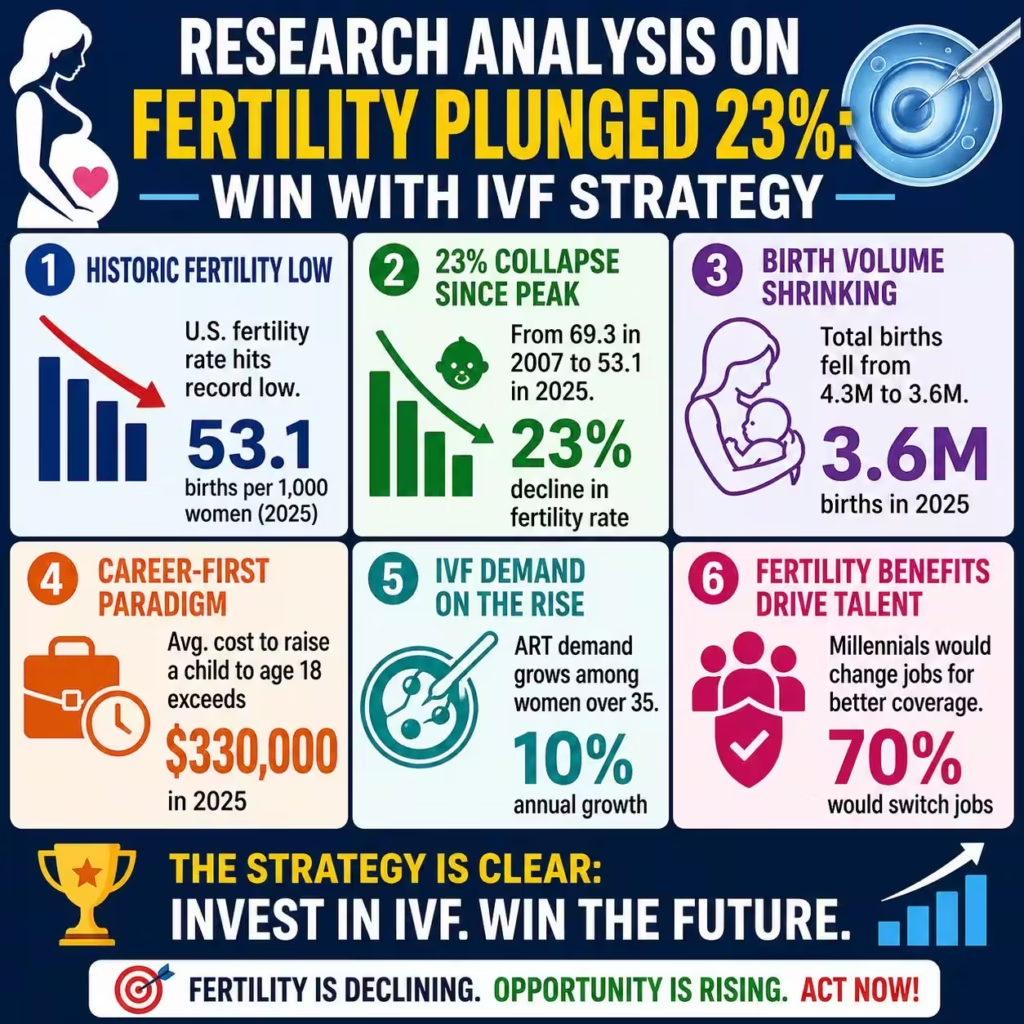
America’s overall fertility rate has plummeted to a record low of 53.1 births per 1,000 women aged 15 to 44, representing a critical inflection point for the healthcare economy. This provisional data from 2025 confirms the third consecutive year of decline, signaling a permanent shift in consumer behavior rather than a temporary lull. The primary pain point is not merely the one percent annual drop, but the 23 percent collapse from the 2007 peak of 69.3. Your healthcare enterprise must recognize that the total volume of births has shrunk from 4.3 million to just 3.6 million in less than two decades. This shrinkage creates a massive vacuum in obstetric revenue and pediatric patient pipelines that will persist for the next 20 years.
The analysis reveals a “striking story” of women intentionally waiting longer to start families, with birth rates for teenagers aged 15–19 dropping by 7% in a single year to 11.7. Conversely, women aged 30–34 and 40–44 are the only demographics showing marginal increases in fertility, yet these gains fail to offset the double-digit declines in younger cohorts. High-authority analysis suggests that the Great Recession’s economic uncertainty has evolved into a structural “career-first” paradigm. In 2025, the average cost to raise a child to age 18 has eclipsed $330,000, creating a financial barrier that simple incentives cannot breach. This article details how B2B entities can pivot toward high-margin fertility preservation and late-stage maternal health to capture this shifting market.
Carethix Critique: Addressing the Risks and Strategic Gaps
Carethix issues a stern critique of the current healthcare response to the CDC’s 53.1 fertility benchmark, identifying a dangerous reliance on legacy obstetric models. The industry is ignoring the 81% decline in teen births since 1991, which previously served as a reliable, albeit socially complex, volume driver for safety-net hospitals. We identify a critical risk in the “wait and see” approach, as the 16 percent total birth volume drop since 2007 is now impacting the labor market and payer mix. The gap between desired family size and actual outcomes is widening because of a lack of affordable, integrated reproductive technology. Most B2B health plans still treat IVF and egg freezing as elective “add-ons” rather than essential retention tools for a talent pool that is increasingly childless.
Furthermore, the “baby bust” creates a massive downstream risk for long-term tax bases and healthcare reimbursement stability. By 2033, the CBO projects that annual deaths will exceed annual births, making net immigration the sole driver of U.S. population growth. This demographic imbalance will strain the ratio of working-age payers to Medicare beneficiaries, which is projected to fall from 2.8:1 in 2025 to 2.2:1 by 2055. Current healthcare systems are ill-prepared for this “graying” of the patient population while their neonatal units sit at 60% capacity. The failure to consolidate maternity services now will lead to catastrophic overhead losses as birth volumes continue their downward trajectory toward the 50.0 floor.
| Related Analysis: Aspirin 80% Lifetime Risk Pain: Unlock Targeted Value UnitedHealth Group $1.5B AI Cost Drag: Unlock Scalable Gains Is 24-Month Tzield Delay Hiding Bigger T1D Failures? |
Strategic Solutions for the Fertility Crisis
To combat the revenue erosion caused by the 53.1 fertility rate, B2B healthcare providers must decisively expand into the “Longevity and Preservation” market. Organizations should urgently convert underutilized labor and delivery units into high-margin In-Vitro Fertilization (IVF) and Preimplantation Genetic Testing (PGT) centers. Statistics show that while overall births are down, the demand for assisted reproductive technology (ART) grows by 10% annually among women over 35. Smart operators can capture this demographic by offering bundled “Family Formation” packages that include egg freezing, genetic counseling, and concierge maternity care. This shift wisely prioritizes high-value clinical interventions over traditional high-volume, low-margin births.
Corporate health consultants should also strongly advocate for “Fertility-as-a-Benefit” (FaaB) integration within standard employer health plans. Data indicates that 70% of millennials would change jobs for superior fertility coverage, making this a powerful B2B recruitment lever. By providing managed fertility benefits, employers can sharply reduce the risk of “multiple gestations” and expensive NICU stays by 50% through single-embryo transfer protocols. Implementing a 24/7 Nurse Care Manager system for fertility patients can increase workplace efficiency by 60% by reducing the stress associated with infertility. These solutions convert a demographic crisis into a specialized, highly profitable service line.
Finally, healthcare systems must aggressively diversify their revenue streams by investing in pediatric-to-geriatric transition services. Since the 2025 data shows fewer children entering the system, the focus must shift to maximizing the “lifetime value” (LTV) of each existing patient. This involves expanding pediatric chronic disease management and behavioral health services, which are seeing a 15% increase in demand despite lower birth rates. By integrating these services, you ensure that the shrinking number of children generates higher clinical engagement and revenue per capita. This proactive re-alignment strategically secures your financial position against the shrinking domestic birth market.
Prevention Steps for Future Demographic Stability
Preventing a total demographic collapse requires a fundamental overhaul of the “Work-Life” architecture within the U.S. corporate ecosystem. B2B leaders must implement “Parental On-Off Tracks” that enable high-performing employees to flex their career intensity without losing seniority or pay. Research from WTW shows that 84% of employers are planning to enhance leave programs by 2026 to combat the talent shortage. You must lead this trend by offering a minimum of 16 weeks of fully paid parental leave to all genders. Standardizing these benefits reduces the “opportunity cost” of childbearing, which is currently the #1 deterrent for women aged 25–29.
Digital health integration is another critical prevention step to mitigate the impact of environmental and lifestyle fertility stressors. We recommend deploying AI-driven fertility tracking and telehealth platforms as a standard part of the corporate wellness stack. Exposure to air pollution and rising temperatures has been linked to a 6% increase in stillbirth risks, making remote maternal monitoring essential. These tools empower employees to optimize their reproductive health windows before age-related decline begins at 35. By investing in “preventative fertility,” you reduce the future need for expensive, late-stage clinical interventions that strain insurance pools.
Furthermore, stabilizing the housing-to-income ratio is a non-traditional but necessary “healthcare” prevention step. Healthcare B2B entities should consider “Employer-Assisted Housing” (EAH) programs to help younger staff achieve the financial stability required for family formation. In 2025, median home prices are nearly 5 times the national median income, a gap that directly correlates with the 23% fertility decline. Offering rent subsidies or mortgage counseling can accelerate the timeline for first-time parents who are currently waiting until their mid-30s. Addressing these social determinants of health is the only way to reverse the downward trend toward a sustainable 2.1 replacement rate.
Carethix Key Takeaway
The 53.1 fertility rate is not a temporary statistic; it is a permanent structural alarm for the U.S. healthcare economy. You must immediately pivot from high-volume obstetric models to high-value fertility preservation and “graying” population services. Failure to adapt to the 3.6 million birth reality will cause stranded assets and unsustainable overhead in maternal care. The future belongs to B2B leaders who treat family building as a managed clinical asset rather than a personal choice. This is your final warning to restructure your patient pipelines before the 2033 population crossover occurs.
Carethix asserts that any executive ignoring the $330,000 “child-rearing barrier” is complicit in their organization’s eventual obsolescence. We view the current obsession with traditional L&D unit maintenance as a toxic “sunk cost” fallacy that drains capital from high-yield longevity markets. You cannot “wait out” a demographic winter; you must engineer a system that thrives in a post-natal economy. Those who fail to integrate aggressive fertility-as-a-benefit (FaaB) strategies today will find their recruitment pipelines frozen by 2030. Stop viewing these record-low figures as a social trend and start considering them as the most significant financial risk to your 10-year EBITDA.
FAQs:
Why has the U.S. fertility rate crashed to 53.1 births per 1,000 women, and what does it signal for healthcare revenue?
It signals a structural demand collapse, and healthcare systems still relying on outdated maternity volume models risk severe long-term revenue erosion.
How damaging is the 23% fertility decline from the 2007 peak of 69.3 for hospitals and pediatric networks?
A 23% drop means shrinking patient pipelines, and leaders who ignore diversification now are effectively planning for underused assets later.
Can the $330,000 child-rearing cost be the real reason younger Americans delay parenthood?
Yes, because until affordability is addressed, most symbolic incentives will fail against such a massive financial barrier.
Why are neonatal units sitting at 60% capacity while systems keep funding legacy obstetric infrastructure?
This reflects poor capital allocation, and executives should urgently convert excess capacity into higher-margin fertility and longevity services.
How serious is the warning that deaths may exceed births by 2033 for the U.S. economy and Medicare base?
It is a major demographic red flag, and failing to prepare for fewer workers supporting more retirees is strategic negligence.
Reference – The real reasons Americans aren’t having babies anymore as fertility rate plunges again


